How MEC reduced plan costs by 12% — without changing networks or cutting employee benefits
Key Results
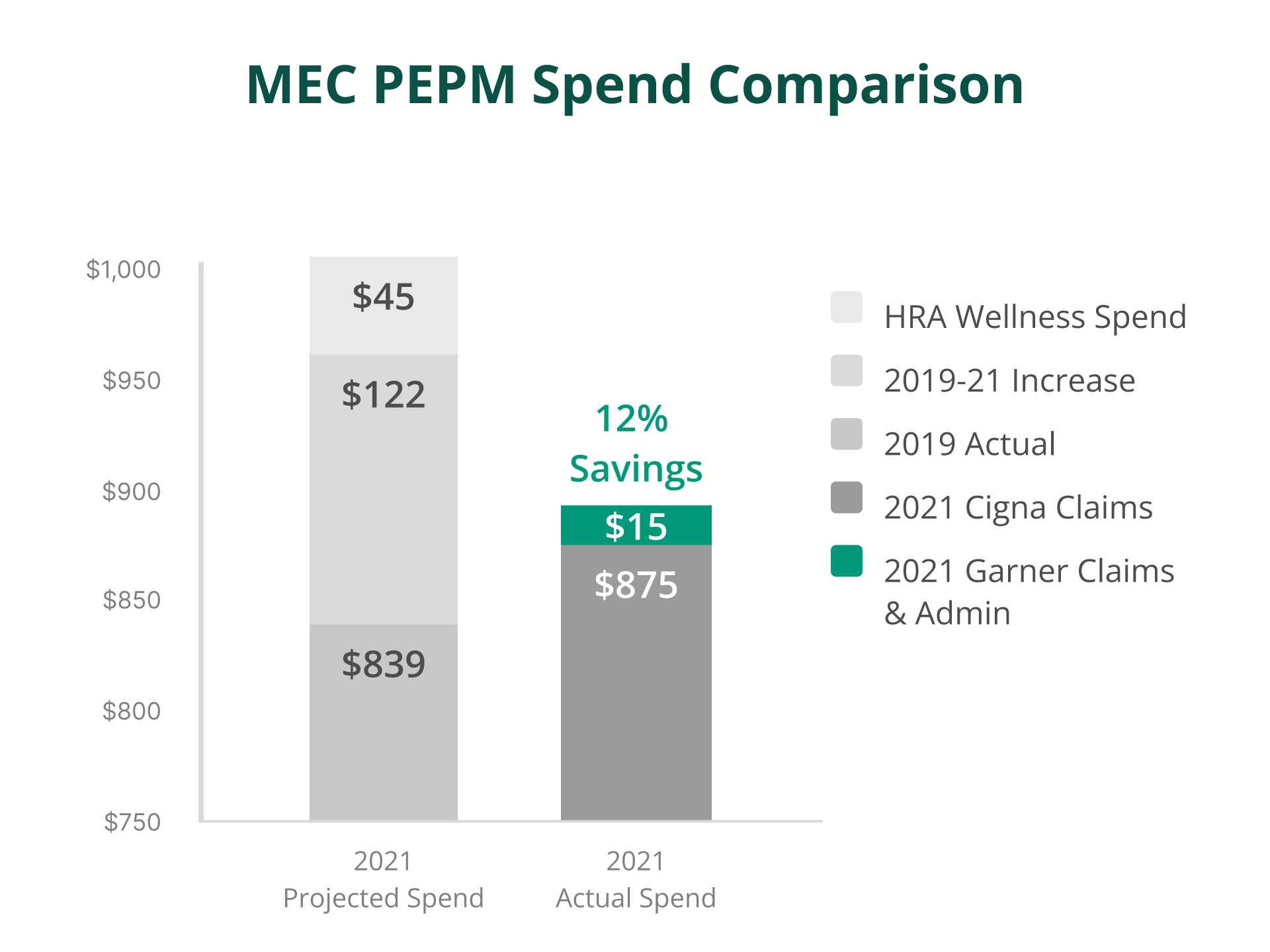
12%
first-year reduction in total claims PEPM
$116
PEPM saved on plan costs — net of all program costs
47%
of employees enrolled in Garner in year one
MEC faced a familiar problem: healthcare costs rising with no good options except cutting benefits or shifting costs to employees. By layering Garner on top of their existing plan — with no network changes — they drove a 12% first-year cost reduction and gave their workforce richer benefits at the same time.
Background
Metal Exchange Corporation (MEC) is a large, self-funded metals manufacturer. As a self-insured employer, MEC bears direct financial responsibility for its healthcare claims — making every renewal a high-stakes financial decision for both the company and its employees.
Going into renewal, MEC had been running a wellness incentive program tied to its HRA. It wasn't delivering meaningful results. Meanwhile, healthcare costs were rising with no sustainable path forward — and employee attrition was making it harder to absorb the trade-offs.
The challenge
MEC faced an unsustainable upward trend in healthcare costs, limited options to manage its spend without cost shifting to employees, and high levels of employee attrition.
The solution
MEC shifted funds from an underperforming wellness program to Garner to ultimately lower total claims spend, deliver a richer benefit offering and provide a better member experience.
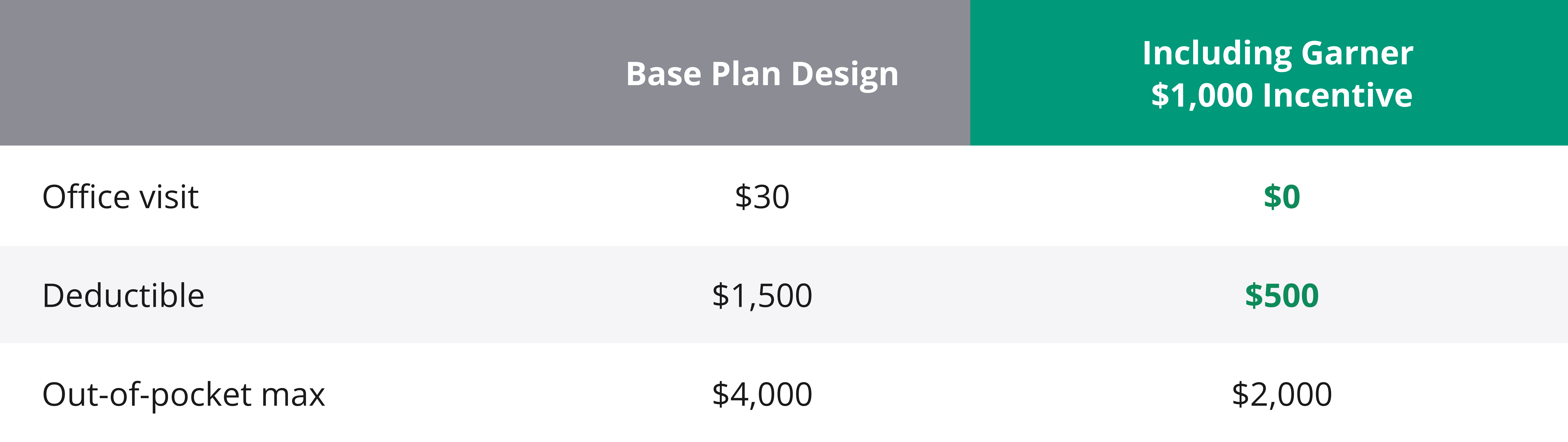
MEC was able to keep its existing plan design and network with no changes. Garner was simply layered on top. The Garner incentive gave members $1,000 to pay for out-of-pocket medical expenses when they engaged with Garner and saw top-performing in-network doctors.
The results
In year one, 47% of employees signed up for Garner. Of those, 72% received at least one recommendation for a provider. As members received higher-quality care, they experienced better outcomes and lowered their out-of-pocket medical costs by 11%. This was a 22% decrease compared to the overall market trend.
The total actual claims PEPM was reduced by 12%, resulting in an annual cost reduction of $736K. These savings were generated as a result of members seeking higher-quality providers, which led to lower costs and better outcomes, as well as overall cost reductions on medical plans.